Identifying the specific type of adverse food reaction and its underlying causes are key to determining effective management and restorative strategies.
The U.S. Food and Drug Administration (FDA) has reported that every year, millions of Americans experience allergic reactions to foods ranging from mild to severe life-threatening, anaphylactic shock. Frank King Jr., ND, DC, founder and owner of North Carolina-based King Bio, manufacturer of the SafeCareRx line of multi-potency homeopathic formulas for natural health care providers, stated that, “food allergies are a growing food safety and public health concern that affect an estimated four to six percent of children in the United States.1,2 According to Tamara Duker Freuman, MS, RD, CDN, food allergies affect from one to four percent of United States adults,” he said. However, other experts such as Aimée Gould Shunney, ND and Nordic Naturals advisory board member, pointed out, “This is very difficult to quantify as many food allergies go undiagnosed, and many food sensitivities and intolerances are never even considered.”
Incidences are on the Rise
The rate of diagnosed food allergies and sensitivities are becoming more prevalent. In 2008, the Center for Disease Control (CDC) published a study that noted an increase of 18 percent from 1997-2007 in the number of young people under 18 experiencing these issues.3 In 2013, another CDC study showed that food allergies among children increased from 3.4 percent in 1997-1999 to 5.1 percent in 2009-2011.4 However, Jacob Teitelbaum, MD, medical director of the Practitioners Alliance Network, suspects that this understates the problem.
What factors are contributing to the increase? “The evidence is mounting (at least among natural health researchers),” Dr. King said, “that the huge increases seen across the board in food allergies and food intolerances are due to multiple factors that cumulatively compromise the immune system. I see many causes, all contributing to the situation, like dominoes falling, cascading one after another.” He added that, “In addition to the known stressors of modern life with our fast-paced lifestyles, we also have the burden of unseen stressors, such as GMO (genetically modified organism) foods, X-rays, microwave radiation (cell phones, Wi-Fi) and EMFs, which make this a challenging environment for those seeking optimal health.”

Genetically modified (GM) foods and human genetics may factor into the equation. Dr. John Hahn, DPM, ND, staff physician at Priority One Nutritional Supplements Inc. in Washington pointed to a “reasonable correlation between the allergies and the genetic modification of our foods over the years. Beginning in 1996, bacteria, virus, and other genes have been artificially inserted into the DNA of soy, corn, cotton seed and canola plants,” he said. “These unlabeled genetically modified foods carry a risk of triggering life-threatening allergic reactions. In March of 1999, researchers at the York Laboratory in Great Britain were alarmed to discover that reactions to soy had skyrocketed by 50 percent over the previous year. Genetically modified soy had been recently entered into the United Kingdom from U.S. imports and the soy used in this study was largely genetically modified.”
With respect to human genetic factors, a connection for peanut allergies in particular has been investigated. “A survey of 622 families with probands of peanut allergy in the United Kingdom noted an increased prevalence of peanut allergy in succeeding generations,” said Dr. Hahn.
Dr. King denoted a link between heavy metals, candida albicans and food intolerance reactions.
“Heavy metal toxicity goes hand-in-hand with candida albicans overgrowth5,6 and both lead to a host of symptoms affecting digestion and more. When candida invades and compromises the walls of the intestines, large particles of protein slip into the bloodstream, causing allergic reactions. Candida overgrowth and general toxicity stemming from poor lifestyle and dietary choices are both factors in faltering immune systems, resulting in food intolerance reactions, including those that affect the brain. “In fact,” he said, “modern researchers call the gut the second brain.7 The evidence for this connection has been persuasively outlined by Natasha Campbell-McBride, MD, in her book, Gut and Psychology Syndrome.”8
Adam Killpartrick, DC, CNS, chiropractor and nutritionist at Suncook Valley Chiropractic in New Hampshire described “impaired digestive health such as mucosal barrier or permeability issues, hypocholorhydria and lack of adequate bacteria in the gut,” as main causes. Additionally, “the toxic, processed foods, prescription drug use and alcohol consumption, have contributed greatly to the impairment of optimal digestion and has led to excessive immune responses to specific foods,” he said.
Dr. Shunney presented a host of lifestyle-related causes for food sensitivities. “Our bodies are burdened with processed foods that are often low in nutrition and high in pesticide residue, while we sleep less, work more and enjoy less down time,” she said. “We experience widespread exposure to environmental chemicals every day in our air, food and water. Our proverbial shopping carts are full, and I think this figures in substantially when we look at a generation of people who seem to be unable to eat many things that their parents and grandparents ate without issue.”
What are the Differences?
How do you determine whether your patient is dealing with a food allergy, intolerance or sensitivity? Dr. Shunney suggested it’s important to “differentiate between these conditions since many patients—as well as professionals—use these terms interchangeably when, in fact, they are quite different.”
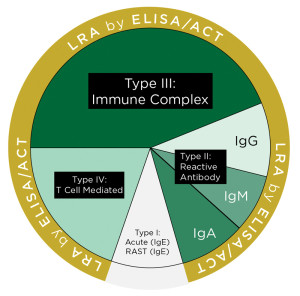
The National Institute of Allergies and Infectious Diseases (NIAID) defines an allergic reaction to food as one in which the immune system responds to food as a threat. Upon first exposure to a food, the body makes IgE antibodies to the allergen, which attach to mast cells and basophils.9 These IgE-mediated immune system responses are typically acute (within two hours) to food exposure and can result in anaphylaxis. According to the FDA, the top eight most common food allergies or intolerances accounting for 90 percent of adverse reactions in the United States are milk, eggs, fish, crustacean shellfish, tree nuts, peanuts, wheat and soybeans. The primary reported food intolerances in the U.S. identified by the NIAID are lactose, food additives, gluten, food poisoning and histamine toxicity.10
A “food intolerance,” explained Dr. Teitelbaum, “represents having symptoms caused by eating a problematic food and can occur from a wide array of causes.” Clinically, he has found that “food sensitivities are associated with three main problems, which often occur in combination: 1) The first is the incomplete digestion of protein caused by inadequate digestive enzymes or stomach acid. The former largely caused by food processing destroying the enzymes and food, which help digestion. The latter by the excessive use of acid blocking medications as well as aging; 2) Leaky gut (increased ball permeability) caused by candida or other infections and decreased healthy gut bacteria from antibiotics and excess sugar; and 3) Adrenal fatigue.”
Dr. Shunney described a food intolerance as “a non-immunological adverse response to certain foods because you lack what you need to digest that food, i.e. lactose intolerance. Food sensitivity,” said Dr. Shunney, “is a non-allergic adverse response (no IgE present),” to a food. “Symptoms tend to be chronic and more delayed in onset (up to 72 hours), making them more difficult to diagnose. Food sensitivities can occur due to eating a food too frequently, poor gut health, stress, nutrient or enzyme deficiencies and other causes.”
Testing and Diagnosis
“Identifying and eliminating problem foods is paramount and testing should be considered,” said Dr. Shunney. “Physicians diagnose immediate-response allergies by measuring IgE antibody levels via a positive skin prick or blood test. Food sensitivities/intolerances can be the toughest to determine since they can cause immediate and delayed responses, and like delayed-response food allergies, they can cause a wide variety of symptoms. Further, since this type of reaction is not an allergy, per se, IgE and IgG antibody levels will be normal and therefore, your doctor will tell you that you have no food allergies.”
Mischelle Hall, operations manager of Virginia-based ELISA/ACT Biotechnologies noted that “other approaches to food sensitivity testing, such as IgG testing, provides only part of the immunologic picture. With IgG testing,” she said, “only the presence and amount of antibody is measured. There is no way to determine which of those antibodies detected are provoking symptoms and which are protecting the patient. A good analogy is measles. If you have had the measles you have antibodies to the measles. That does not mean you currently have the measles or have symptoms of the measles. Only by directly measuring lymphocyte change after exposure can you be certain that the item is triggering symptoms.”
“ELISA/ACT Biotechnologies founder Russell Jaffe, MD, PhD has developed an ex-vivo cell culture method that allows direct observation, under a microscope, of live lymphocytes as they are exposed to as many as 504 different foods and chemicals. The test is called LRA (Lymphocyte Response Assay) and can be used to detect delayed hypersensitivities to foods, food colors, preservatives, environmental chemicals, molds, toxic mineral/metals and more,” said Hall. This test is available exclusively through ELISA/ACT Biotechnologies for licensed health care practitioners.
Several practitioners have had success utilizing an elimination diet as a reliable diagnostic method. “An elimination and challenge diet (ECD) will uncover even the subtlest of delayed-response food allergies, food sensitivities and food intolerances,” said Dr. Shunney. She has developed a specific implementation method that she uses and follows. Adjusting as needed as a patient progresses.
Dr. Killpartrick has combined a rotational elimination diet with tests from ALCAT, Alletess and Genova Diagnostics. “I’ve also had great success with patients that I simply implement an elimination diet removing the top eight allergens for a period of time and gradually reintroduce to assess reactions,” he said.
Jim Fox, DC MACN, co-owner of Doctors Nutrition, LLC in Mississippi expressed, “The most effective and specific testing that we have found clinically is the ALCAT blood test.” The ALCAT tests by Cell Science Systems are non-IgE mediated tests for foods, chemicals and other substances. Dr. Teitelbaum additionally recommended the use of applied kinesiology for diagnosis when done by a skilled practitioner.
Alleviating Food Reactions
Dr. Hahn at Priority One Vitamins supports the naturopathic/holistic viewpoint that “allergies are often associated with weak adrenals, immune and digestive functions. Our company’s approach to the food sensitivity issue is holistic in that we look at the whole body’s reaction to an antigenic threat and try to establish homeostasis by supporting healthy adrenal function, digestive enzyme capacity and appropriate gut probiotics,” he said. “We have specific enzyme products such as Gluten Resolve which addresses individuals that have gluten sensitivities and other food sensitivities by combining a unique ingredient profile that addresses various food components in order to reduce the antigenic capacity to create food allergies.”
Dr. Hahn additionally suggested that individuals who have food intolerances would benefit from taking a multi-enzyme product to aid the breakdown of food into easily absorbed and digested particles. “Our two phase digestive enzyme, Enzy-Gest supports healthy digestion; its sister formula Hypo-Gest is a higher potency alternative. Our Gastri Gest is a plant based digestive enzyme suitable for vegetarians. Physicians can select from a vegetarian base or glandular base product.”
Dr. Killpartrick also advocated the use of digestive enzymes. “This is especially true for certain proteins which pose a problem such as those found in gluten and dairy,” he said. He also recommended a diet specific to food intolerances as essential along with gut repair. “Once you optimize the diet specific to the patient’s needs, then you repair the gut. Repair includes nutrients such as glutamine for integrity, curcumin for inflammatory support and probiotics for bacterial balance.” Dr. Fox agreed, “You have to reestablish the integrity of the endothelium of the GI (gastrointestinal) tract, thus changing the permeability and reducing the influx of undigested food particles into the blood stream.”
Dr. Teitelbaum has incorporated “plant-based digestive enzymes along with adrenal support while treating candida and other gut infections to help reverse the dysbiosis.” Complete gest or Similase digestive enzymes along with Adrenal Stress End are products he has used, in addition to an enteric coated probiotics such as Probiotic Pearls. “If not enteric-coated, the stomach acid will kill most of the probiotics,” he said.

In addition to an elimination diet, Dr. Shunney uses supplements “to help decrease inflammation, modulate the immune system, heal the gut and manage persistent symptoms.” She consistently recommends an omega-3 fish oil. “Nordic Naturals ProOmega is a high-quality choice with Nordic Naturals Algae Omega being a great vegan alternative. Omega-3 fats from fish and algae are suitable for infants, children, pregnant women, and adults at all stages of life. I would recommend 1,500-2,000 mg of EPA and DHA (which equals three to four soft gels of ProOmega) daily for adults to support immune function and optimal cellular health. GLA from borage oil is another supportive essential fat. Two soft gels of ProEPA with Concentrated GLA (another Nordic Naturals product) provide about 1,100 mg of EPA and DHA, along with about 250 mg of GLA. Together, EPA, DHA and GLA can positively impact cellular stress,” she said. “Turmeric, I-glutamine, digestive enzymes and a potent pre- and probiotic are some of my other common recommendations,” Dr. Shunney added.
The health essentials Dr. King considers are outlined in his book, The Healing Revolution: Eight Essentials to Awaken Abundant Life, Naturally. “Beyond those,” he said, “homeopathic medicine effectively reduces allergic and intolerance responses to foods, and also reduces candida overgrowth, and helps the body excrete heavy metals.”11 Dr. King’s SafeCareRx line of products offers eight formulas related to food allergies and intolerances for: dairy, nuts & seeds, grains & gluten, shellfish & seafood, eggs & meat, fruits & vegetables, food chemicals and nightshades.

“Homeopathy offers great hope for those with food intolerances and food allergies, although my protocol is different,” he added. “Our allergy products work to actually correct the allergy and desensitize the patient so he or she needs less over time, and may eventually not need the products at all. For those with life-threatening allergies, he advises medical supervision and with patients with strong allergic reactions, advises going very slowly with his contemporary homeopathic medicine.
Another approach which aids in desensitizing people to foods is the Nambudripod Allergy Elimination Technique (www.naet.com) “which can be learned easily by most health practitioners,” said Dr. Teitelbaum. “I routinely see food sensitivities/intolerances resolve with NAET,” he said. Treating the adrenal and digestive issues in conjunction make it less likely for the sensitivity to recur.
In summary, Dr. Killpartrick stated, “The subject of food intolerances is dictated by two major factors: internal functionality and external food choices. When both are addressed, true progress can be made. But both factors need to be addressed. Simply removing gluten without addressing the damage that gluten may have done on the gut limits the potential for success.”
Future Outlook
When it comes to food reactions, “These are a major cause of the autoimmune epidemic, which I think will be the most common illnesses in this century” predicted Dr. Teitelbaum. Dr. King finds “genomics and our recent understanding of the microbiome within to be a fascinating, empowering and exciting new frontier,” he said, citing an encouraging new study using peanut protein and probiotics.12
From Dr. Hahn’s perspective, he believes that “as a result of the increased number of individuals experiencing both food intolerance, food allergies and environmental allergies that the options for treatment utilizing natural medicines will be increasing. I believe that manufacturers will be exploring ways to stabilize mast cells and basophils in order to prevent release of histamine, bradykinin, and other pro-inflammatory substances that result in symptoms of allergies,” he concluded.
References:
1 Branum AM, Lukacs SL. Food allergy among U.S. children: trends in prevalence and hospitalizations. NCHS Data Brief. 10:1-8, 2008.
2 Liu AH, Jaramillo R, Sicherer SH, et al. National prevalence and risk factors for food allergy and relationship to asthma: results from the National Health and Nutrition Examination Survey 2005-2006. J Allergy Clin Immunol. 126(4):798-806.e13, 2010.
3 www.cdc.gov/media/pressrel/2008/r081022.htm.
4 www.cdc.gov/nchs/databriefs/db10.htm.
5 www.ncbi.nlm.nih.gov/pmc/articles/PMC1951024/.
6 http://onlinelibrary.wiley.com/doi/10.1002/jobm. 200510609/abstract.
7 www.psychologytoday.com/articles/201110/your-backup-brain.
8 Campbell-McBride, Natasha, MD, Gut and Psychology Syndrome, Medinform Publishing, 2010.
9 www.niaid.nih.gov/topics/FoodAllergy/understanding/Pages/allergicRxn.aspx.
10 www.niaid.nih.gov/topics/FoodAllergy/understanding/Pages/foodintolerance.asp.
11 www.complementarytherapiesinmedicine.com/ article/S0965-2299%2898%2980025-3/abstract?cc=y.
12 http://time.com/3685910/peanut-allergy-cure/.
For More Information:
Dr. Jim Fox, (228) 897-0070
Dr. Adam Killpatrick, (603) 435-6600
Dr. Jacob Teitelbaum, (410) 573-5389
ELISA/ACT Biotechnologies, (800) 553-5472, www.elisaact.com
King Bio, (800) 543-3245, www.kingbio.com
Nordic Naturals, (800) 662-2544, www.nordicnaturals.com
Priority One Nutritional Supplements Inc., (800) 443-2039, www.priorityonevitamins.com













