People come to you because something is hurting. Beyond signifying dire health straits, there are effective natural ways to help manage the aches.
A perennially funny joke is when a patient says to the doctor, “Hey doc, it hurts when I do this.” The doc’s recommendation is simply, “Well, don’t do that.”
If only it were that simple—the world would indeed be a much, much different place.
Of course, the temporary fireworks pain that bursts from a momentary collision of the knee or elbow or toe against a piece of furniture notwithstanding, pain that persists is a top reason why patients are sitting in your exam room.
Practitioner AnnAlisa Behling, ND with four practices in Michigan, observed that typically, people seek out help after experiencing pain for a more chronic duration. It may already be months before what they thought was just an acute, temporary issue has become more persistent. In her practices, she noted that the most common pain points are joint aches, like arthritis, or degenerative issues (bone on bone). “Headache pain, low back pain (muscular, nerve and spinal issues), gastrointestinal (GI) pain are all next in line as well. For some women, endometriosis, ovarian cyst or uterine fibroids can also create such pain that they are debilitated for a day or two around those acute ‘attacks,’” she elaborated.
Additionally, pain can come in the form of nociceptive or neuropathic, or mixed types, added Robert Kachko, ND, New York-based InnerSource Health, and president of AANP (American Association of Naturopathic Physicians). Quite frequently, he emphasized, “there is also a central component once pain becomes chronic, impacting pain perceptions.” Factors like mindset, hyper-vigilance, catastrophizing, pain expectation, environment, lifestyle and genetics among others contribute to the pain profile the patient presents.
And, as with Dr. Behling, Dr. Kachko said that the most common pain conditions that bring people to the doctor are low back pain, arthritis and headaches.
Because talking about pain is often the opener during the consultation, questions can make all the difference in arriving at the correct diagnosis and treatment. These questions are critical due to the widespread disparity in pain perceptions, Dr. Kachko explained.
Dr. Behling agreed, adding that pain can be expressed very uniquely in each person and thus is very subjective. For example, she offered, think of childbirth: there are women who go the entire labor with no pain medications and those who need something within the first hour of contractions.
Interestingly, she explained, men and women experience pain differently from one event to the next. In 1995, a major review of the research literature on pain and gender found that women experience more pain (intensity) than men overall but also have a lower threshold and tolerance to “experimental” pain, including mechanical, thermal and electrical. But in 2019, a study published in Current Biology, explained that women can handle pain better than men based on “the memory of pain.” In other words, she clarified, “re-exposure to the same experience of pain resulted in pain hypersensitivity.”
Dr. Behling attempts to have the patients explain the pain they are experiencing in a specific manner. Questions include: Where is the direct pain, does it radiate somewhere or progress from mild to severe (e.g., migraines); when does the pain occur? Is it continuous, come and go, how long does it last? Is it triggered by anything (movement, food, deficient sleep, stress, etc.)? How bad is the pain on a one to 10 pain scale regularly, and what is the worst pain you have experienced? Is the pain debilitating and/or does it alter your quality of life and if so how (i.e., sleep, work, play)? Does it affect your mood or personality? How long have you been experiencing the pain? When did it begin, was there an original injury or perhaps a degenerative issue?
Depending on the pain profile garnered by these responses, fellow practitioners may call for imaging (e.g., Ultrasound, X-rays, MRI, CT, etc.) for further discernment and clarification. Dr. Kachko ‘s viewpoint is that every practitioner must take a biopsychosocial approach.”
Bio: Biological or biomedical, which considers bodily structure and function to ascertain the physical source of pain, may emanate from trauma or another type of physical lesion, inflammation, infection or immune system impacts as with autoimmune pain disorders. Treatment may include recommendations for medications, surgery, exercise, injections or a myriad of other techniques.
Psycho: Psychological. “While it’s never true that pain exists only in the mind, the mental-emotional aspects of who we are do always play a strong role in how much we are impacted by our pain,” Dr. Kachko explained. That said, he pointed out, emotional pain (stress, anger, frustration, anxiety, etc.) is very real and can add to the experience of one’s physical pain. Similarly, reduction of emotional pain can reduce the sensation of physical pain. “If the biomedical approach aims to understand the physical source of a person’s pain and eliminate it directly, the psychological approach (which is completely complementary) aims to understand and address the suffering that we experience when we feel discomfort,” he added.
Social: The relationships and interactions that we have, no matter what kind they are, impact in either helping to feel better or to feel worse. In other words, he noted, the environment within which your patient experiences his or her pain matters as well.
“Every provider must consider all three components for every person dealing with pain,” he said.
Common Pain Resolutions
As mentioned, the most common pain complaints are joint health related, back/muscle, headache and GI. And as you know, the priority is to assign a protocol that manages the pain before other actions can be taken to deal with the emanation or cause. Drs. Behling and Kachko offer their thoughts on proper pain management protocols.
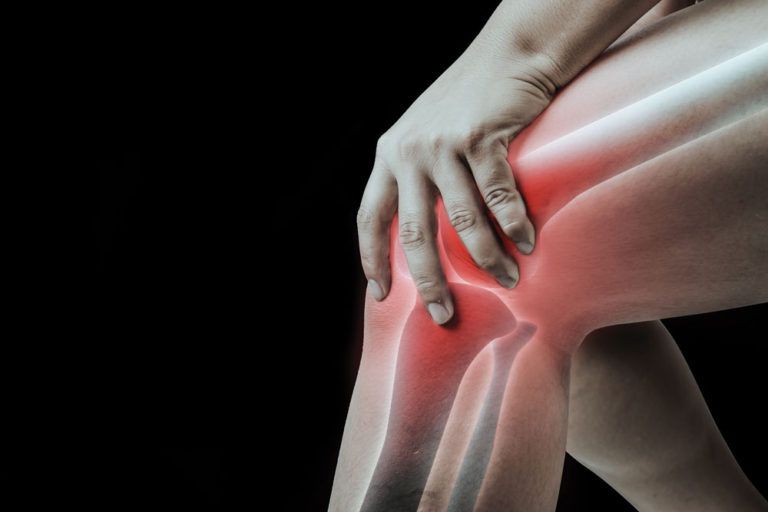
Joint Pain
According to Dr. Behling, osteoarthritis (OA), a degenerative joint disease, is the most common form of arthritis affecting more than 20 million people older than 45 in the United States. However, currently, no specific treatment exists to halt the progressive cartilage degeneration of osteoarthritis or to repair the damaged cartilage. “With OA, this pain is typically more than an acute issue and people experience a progression in pain as the joint regions degenerate so [they] should focus on anti-inflammatories as well as supportive supplements,” she emphasized.
Supplements she recommends include:
Turmeric: This popular ayurvedic herb has more than 5,000 studies demonstrating anti-inflammatory, antioxidant and immune-modulating abilities as well as the ability to help reduce connective tissue inflammation and therefore provide some pain relief.
An attractive reason to add turmeric and lessen use of NSAIDs (nonsteroidal anti-inflammatory drugs) is the results of an RCT (randomized controlled trial), which Dr. Behling finds compelling. The RCT compared the effects of curcuminoids (30 mg, 3 times/day) to the NSAID diclofenac (25 mg, 3 times/day) on COX activity in the synovial fluid of the joints in patients with osteoarthritis. The researchers found that the turmeric was equal in anti-inflammatory and pain potential as the NSAID.
Boswellia serrata: Research shows that boswellic acid from this ayurvedic herbal mainstay can deter the formation of leukotrienes, which are pro-inflammatory molecules.
Ginger: This herb has been shown in some studies to be as effective as ibuprofen for reducing discomfort related to arthritis via an anti-inflammation pathway.
Omega-3 EFAs (EPA/DHA): EPA is highly anti-inflammatory and a good quality high dose of 26,000 mg EFA can help most pain and inflammation by helping maintain prostaglandins.
Hyaluronic acid: HA, known also for skin plumping (beauty), gives synovial fluid its viscous properties preserving joint flexibility, elasticity and hydration.
Glucosamine: This is a nutritional building block for connective tissue and necessary for the production of hyaluronic acid and chondroitin sulfate which support joint comfort and improved mobility.
MSM (methylsulfonylmethane): This naturally occurring source of sulfur in the body is often used in formulations for joint support and circulation, as it is needed to make collagen.
Chondroitin: This is a substance that occurs naturally in the connective tissues; sea cucumber offers a rich source of highly bioavailable chondroitin sulfates.
Collagen: Type II collagen is one of the main proteins in cartilage. “It’s been suggested that taking collagen hydrolysate and other factors can improve the symptoms of osteoarthritis by stimulating your body’s production of joint collagen,” Dr. Behling said.
Cyplexinol: This patented ingredient is a naturally derived, biologically active protein complex consisting of bone morphogenetic proteins (BMPs) which stimulate bone and cartilage growth and fight inflammation. Dr. Behling reported that according to a double-blind, placebo-controlled study, participants consuming Cyplexinol reported a significant decrease in pain and stiffness, and a significant increase in quality of life (QOL) as compared to those treated with placebo.
“Joint pain has always been considered inflammatory (e.g., rheumatoid arthritis) or non-inflammatory (as in osteoarthritis),” stated Dr. Kachko. “However, this is far too simplistic, and most people with chronic joint pain have some degree of inflammation (primary or secondary) which must be addressed. Also, many types of arthritis can have metabolic triggers.”
Back/Muscle Pain
Dr. Kachko believes it is important to teach patients to be as mobile as possible as soon as they can after acute injury. This reduces the likelihood of keeping back pain from becoming chronic. As with most pain, natural anti-inflammatories and anti-spasmodics provide relief. “I also find inversion as well as movement therapies that retrain the posterior chain of muscles to move in unison is essential. Acupuncture works very well in both acute and chronic stages,” he explained.
Dr. Behling will recommend supplements such as turmeric, boswellia, devils claw, bromelain, capsaicin, menthol/methylsalcylate, willow bark as well as Arnica montana and other homeopathics such as aconitum, belladonna, Hypericum perforatum, Symphytum officinale, chamomilla, etc. There are patented products (like Traumeel) which have a complex of homeopathics in it or can use the single remedies.
Adjunct therapies she likes to recommend to patients with back pain are Epsom salts in baths, hydrotherapy and alternating hot/cold, low level laser therapy, ultrasound, acupuncture, pulsed electromagnetic field and massage therapy. Adding yoga will help keep the back strong and supple.
Headache
When patients complain of headache, Dr. Behling likes to see if it can be caused by inadequate or chronic dehydration, which is easily fixed by increasing water consumption. Magnesium is good to take as it “works with muscle contractility, nerve signal transmission and vasodilation and blood pressure regulation, which can help tension and cluster headaches as well as migraines. Use citrate, malate or glycinate for good absorption and to prevent diarrhea if taking in higher doses. You can also eat nuts and seeds high in magnesium,” she advised. Herbs she likes are butterbur, feverfew and willow bark. And, she will recommend acupuncture for headaches, citing a review of 22 studies including more than 4,400 people which found that acupuncture was as effective as common migraine medications.
For migraines, Dr. Kachko asserted practitioners “must consider the impact of food allergens. Most common are wheat/gluten, dairy, citrus, chocolate and hard cheeses. Also, consider food additives and preservatives in highly sensitive people.” He added that paying attention to fortifying the microbiome is important and can have beneficial impact.
Other Pain Management Solutions
Arnica montana, a type of mountain daisy, has been used for centuries as a pain reliever and is one of the most popular homeopathic medicines worldwide, according to Christophe Merville, D Pharm, director of education and pharmacy development, Pennsylvania-based Boiron. Boiron offers Arnicare, a line of over-the-counter products (pellets, tablets, gel, cream and ointment) containing arnica to help relieve muscle pain and stiffness, swelling from injuries and discoloration from bruises.
He described, “Homeopathic arnica is a useful tool in pain management. Alone or in combination with other homeopathic medicines targeting arthritis pain or pain from trauma or overexertion, it allows the patient to address flare ups of pain as soon as they occur, and contributes to decreasing or avoiding the need for stronger, but less safe pain-killers.” Arnicare can be recommended in cases of physical trauma, such as elongations, strains or sprains, or trauma due to repetitive movements, neck or back aches and stiffness due to prolonged bad posture or immobility. It is commonly used to relieve swollen and painful feet from standing or walking for long periods of time.
Merville explained that arnica exerts three therapeutic properties: mild analgesic, anti-inflammatory and anti-ecchymotic. The plant’s main component helenalin, interferes with the regulation of genes coding for many inflammatory mediators at a very low cytosol concentration. This means it reduces swelling and discomfort caused by inflammation. And, among other components, polysaccharides in arnica stimulate phagocytosis and possibly reduce bruising, he added.
Palm fruit bioactive complex (PFBc) is a water-soluble botanical ingredient that was identified and researched by internationally-recognized research groups from the Malaysian Palm Oil Board, MIT, Brandeis University, Harvard-Brigham and Women’s Hospital, Wayne State, and CSIRO, described Kevin L. Ohashi, PhD, CEO, Massachusetts-based Phenolaeis. Palm Fruit Bioactive complex is the water-soluble botanical components isolated from the water stream generated from oil palm fruit processing.
To date, he said, “there are 20 peer-reviewed publications and nine international research awards achieved by the work that two MIT research groups and the Malaysian Palm Oil Board (MPOB) have supported. This non-clinical research, along with human clinical studies, has shown that PFBc activates a wide range of antioxidant pathways. Antioxidant pathways are known to support the immune system, cardiovascular and cognitive health.”
Ohashi further explained that in nonclinical research by MPOB and MIT, changes in gene expression were observed and correlated with various biomarkers that have been associated with assisting in protection of cells and tissues. In addition, the studies have also indicated changes in various immune system biomarkers that may be associated with wellness.
One of the human clinical studies used a 10K run to induce an increased level of oxidative stress in individuals, and supplementation with PFBc for 30 days showed distinct and significant improvements in individual’s antioxidant reserves with trends showing highlights changes in various mind and body biomarkers and mood over placebo controlled groups, making products that contain it a desirable tool to manage pain and discomfort.
According to Mark Faulkner, president, Vireo Systems, Inc., Tennessee, in research conducted at three major university medical centers, the active ingredient in Amino Activ (Alpha-GEE) has been shown to have the same dose-related anti-inflammation properties as ibuprofen, the most commonly used NSAID.
Alpha-GEE is ethyl-[α-[guanido-methyl] ethanoate, what Faulkner described as a unique peptide compound conjugated from various essential and conditionally essential amino acids found in fruits, beans, legumes, leafy green vegetables, root vegetables, nuts, seeds and some meats. The amino acids which form this peptide do not individually have anti-inflammatory properties, but, he emphasized, “when synthesized and conjugated, they form a compound that expresses beneficial effects on inflammation.”
Besides positive clinical outcomes with prostaglandin suppression, Amino Activ and Alpha-GEE have also been shown to support suppression of systemic inflammation markers.
A device called LightSlim, LED light therapy, is now available for practitioners. It is offered in several different models including hand-held as well as hands-free portable units, a stand-alone device with 1,400 LEDs designed to conform to any treatment area, and the first-ever FDA (U.S. Food and Drug Administration)-cleared LED Bed.
The LightStim MultiWave Patented Technology combines four wavelengths—630 and 660 nm red, as well as 855 and 940 nm infrared to help relax tissues and relieve pain. The devices are FDA cleared to temporarily relieve arthritic pain, a variety of minor aches and pains, relax muscles, and increase local blood circulation.
Pain will always be a driving force for patient visits—and the more you can help reveal the type and cause of a patient’s aches, the more immediately he or she can disembark the pain train.
Healthy Take Aways
• Factors like mindset, hyper-vigilance, catastrophizing, pain expectation, environment, lifestyle and genetics among others contribute to the pain profile.
• The most common pain conditions that bring people to the doctor are low back pain, arthritis and headaches.
• Men and women experience pain differently from one event to the next.
• Emotional pain (stress, anger, frustration, anxiety, etc.) is very real and can add to the experience of one’s physical pain.
For More Information:
Boiron USA, www.boironusa.com
LightStim, www.lightstim.com
Phenolaeis, www.phenolaeis.com
Vireo Systems, https://vireosystems.com/






![[The Vitamin Professor Podcast] Lesson 13: Kesum for Cognitive Function, Inflammation & More](https://naturalpractitionermag.com/wp-content/uploads/2025/01/vre-nie-npr-2025-01-podcast-1-300x169.jpg)




