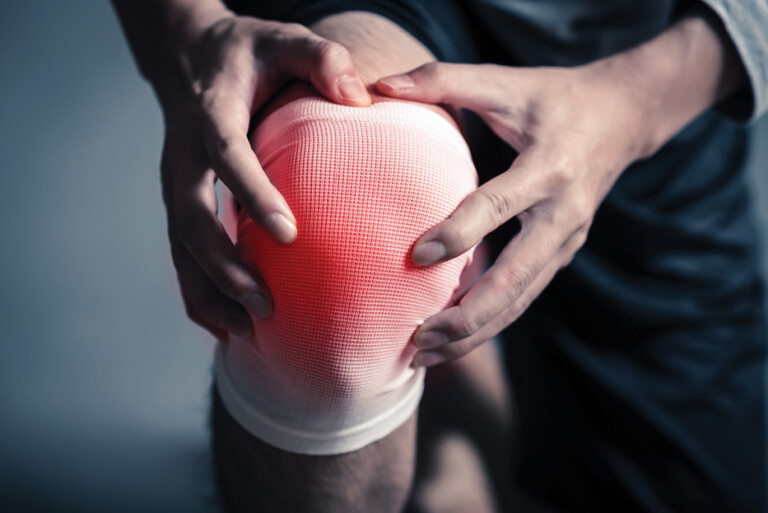
When it comes to pain and inflammation, according to the Centers for Disease Control and Prevention (CDC), about 20 percent of adults in the U.S. are in chronic pain, with much of this stemming from inflammation in the body. Inflammation is the body’s response to invaders or injury, however, the issue becomes when inflammation does not resolve, and becomes a chronic concern. In fact, chronic inflammatory diseases are the most significant cause of death in the world.1 There are nearly as many risk factors as there are chronic diseases, as inflammation and pain can further appear in a variety of mechanisms. Fortunately, while natural and conventional medicine can be helpful, healing is typically of mind-body-spirit related therapies, which need to be explored.
When it comes to mechanisms, one that occurs is that there is an influx of white blood cells and inflammatory cells such as macrophages, lymphocytes and plasma tissues, all of which can then produce cytokines, growth factors, enzymes—all of an inflammatory nature—which contribute to tissue damage and impair factors needed to repair systems.2 In the acute stage (i.e. injury, cut), the body brings in these mechanisms to head and repair, anywhere from a few days to weeks. However, in a more chronic stage, it can affect organ systems or even our musculoskeletal system where if there’s an “overload of debris,” it can get stored and cause pain and other issues.
Another specific mechanism is when arachidonic acid makes prostaglandins, which have a variety of functions, though in this case made during cyclooxygenase (COX) (COX-1 being predominant, COX-2 relating more toward inflammation), which can then increase c-reactive protein (a blood marker for inflammation), leading to chronic inflammation, immunosuppression of IgG (long-term), IgE (allergies), and IgM (immediate reaction), which can contribute to concerns such as rheumatoid arthritis and asthma.3,4
Lastly, reactive oxygen species (ROS) are another type of pro-inflammatory molecule, where oxidative stress occurs when there’s too much ROS and not enough antioxidants.5 This interestingly is metaphorical to what it means to be in balance. In other words, we do need some sort of inflammation in the body, however, when it becomes too much or when ROS becomes out of balance with antioxidants and overall health, pain and inflammation can occur. Further, this stressor on the body can interfere with a variety of other mechanisms, something that needs to be considered when we think of what is the root cause, or underlying issue(s) as described by the patient.
Some risk factors for chronic inflammation is poor diet (especially high in saturated fats, or high sugar), genetics (i.e. MTHFR enzyme malfunction), increasing age, stress, poor relationships (with self and/or others), smoking, alcohol, an acute inflammatory issue (i.e. food poisoning), food allergies or intolerances, environmental toxins, autoimmune disease and other substances. These can cause hormone imbalances, pain, gut issues, migraines and other headaches, allergies, autoimmune disease and chronic obstructive pulmonary disease (COPD) and many people can have one or multiple concerns [each of which may contribute to further decline].2 In this day and age as well, we have access to products, and foods, for example that may not always be the most healthful for us, so it can be more than what we ingest, but what we put on our body from sunscreen to beauty products that can seep through the skin and affect our physiology, commonly known as endocrine disruptors (that can affect our hormones and detoxification systems, which can potentially worsen pain and/or discomfort).
Stress on the body can take a variety of forms, including studies showing that loneliness and lack of community can contribute to greater inflammation, especially in the case of stressor(s). On the mental-emotional sphere, it may even be taken so far as to being with people whom even if someone can’t truly be themselves, or are in unhealthy scenarios, can also be a very lonely feeling.
Common symptoms of chronic inflammation can look like pain and inflammation as discussed, as well as depression, anxiety and mood disorders, chronic fatigue and insomnia [the irony as poor sleep can contribute to many of these symptoms, plus additional stress], constipation, diarrhea, acid reflux, weight gain or loss, and/or frequent infections.2 These symptoms can be alone or work together, hence why it’s important to go through a review of systems while also noting what the patient is most concerned about. Many of these concerns can also overlap into each other as well, so testing and different types of therapies can be helpful in not just assessing the amount of inflammation, but help the practitioner navigate the type of therapy needed for pain and inflammation, as well as any other potential concerns.
Blood tests to consider ordering would be a complete blood count and comprehensive metabolic account, an iron panel (inflammation can show high ferritin), lipid panel (stress can appear as elevated LDL, with inflammation potentially showing an elevated HDL), vitamin B12, c-reactive protein (CRP) and/or hs-CRP, otherwise known as highly sensitive CRP, homocysteine (can tell about their detoxification and metabolizing cycles), ESR and vitamin D 25-OH. It has also been suggested to test fibrinogen, perform a serum protein electrophoresis (SPE) that can show any additional hypoalbuminemia and polyclonal increase in all gamma globulins, as well as and any pro-inflammatory cytokines such as TNF-alpha, IL-1Beta, IL (interleukin)-6, IL-8, though the latter can be more expensive.2 When it comes to more specialized tests, urine, and/or saliva can be more accurate if there’s also a hormonal picture, neurotransmitters if there’s a significant amount of stress, anxiety, and/or depression, stool test or food intolerance test, and/or potentially Boston Heart Tests can be helpful to investigate any abnormal cholesterol, genetic or inflammatory markers as well that could be contributing.
Some of the many therapies available include managing diet and lifestyle as very important, given what we put in is literally what we get out. Helpful tips include a healthful diet with a variety of fruits and vegetables (though may want to be wary of high glycemic fruits and foods in general with inflammation, and especially if there’s blood sugar issues), and aiming for whole foods instead of processed foods or those with many ingredients. Avoiding soda, alcohol, refined carbohydrates, high fructose corn syrup, trans fats and vegetable oils are highly suggested, instead replacing everything with adequate water intake (or green or black tea for polyphenols which helps reduce CRP), high fiber (which can lower levels of IL-6 and TNF-alpha), and adding sesame oil (can taste good on protein sources, and sauteed vegetables), which has been shown to reduce the production of prostaglandins, leukotrienes, and thromboxanes.2 Adequate rest will also be important to help regulate cortisol (stress), such as going to bed before 10:30 p.m., and getting a restful seven to nine hours of sleep. Castor oil packs around the abdomen can be helpful with digestion and overall aiding in gentle detoxification, as well as even as a topical on painful areas. Studies have further shown that having gratitude for who and what’s around us (even ourselves!), has been imperative for reducing pain.6 Mindfulness, yoga or any other form of gentle movement that promotes relaxation can be helpful as well. In addition, finding ways to strengthen other parts of the body (even having gratitude for what our mind and body can do), can also foster positive feelings.
Acupuncture is a great modality to help with pain, as NSAIDS (non-steroidal anti-inflammatory drugs) tend to be the most common used by conventional medicine. When it comes to supplements, herbs even in combination like ginger (inhibits COX-2), Boswellia serrata and curcumin (multiple inhibitions of inflammatory molecules) can be grouped together to act on similar mechanisms as an NSAID. Bromelain, a digestive enzyme, is great when taken between meals to help with overall inflammation (suggested 500 mg).7
Other recommendations can include prolotherapy, a well-taken homeopathy case or perhaps just an acute-related remedy, and even a homeopathic injection as additional options.8 Supplements should also be geared towards what else the person may be experiencing as discomfort can be contributing, as well as considering any mental/emotional support in terms of homeopathy, herbs, cell salts and flower essences (especially the latter which they can use throughout the day). One of my personal favorites is hawthorn, which can reduce any anxiety and good for heart disease, as well as work on the heart emotionally to foster more love and self-care. Likewise, it may be helpful to look at the relationship to themselves, as well as to others. If they feel they need to over-give or haven’t felt happy in a while, it is quite synonymous to their body not being happy either, and strengthening their mind and sense of well-being is just as important as strengthening their body back into health (mind-body connection).
When it comes to pain, there are many different mechanisms and approaches that a practitioner can take, ideally too with the patient’s best interest in mind, and a plan that will fit into their desired lifestyle. Building their foundation with diet and lifestyle will assist in other therapies, as well as ensuring that it’s a mix of decreasing the pain, and as well as treating and strengthening other aspects of their mind and body as they heal. There may not be a “one size fits all,” but we may find that in treating one concern the pain decreases, or conversely by honing in on pain, other concerns may decrease. It’s often a time where the person can truly engage in satisfying activities, good company and perhaps, a chance to get back to a self-care routine (or develop a new one). If they’ve been living with this for a while, it may take some time, but certainly something we can address from each of our areas of expertise and understanding.
References:
1 Rikard SM, Strahan AE, Schmit KM, Guy GP Jr.. Chronic Pain Among Adults — United States, 2019–2021. MMWR Morb Mortal Wkly Rep 2023;72:379–385. DOI: http://dx.doi.org/10.15585/mmwr.mm7215a1.
2 Pahwa R, Goyal A, Jialal I. Chronic Inflammation. [Updated 2023 Aug 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan. www.ncbi.nlm.nih.gov/books/NBK493173/.
3 Simon LS. Role and regulation of cyclooxygenase-2 during inflammation. Am J Med. 1999 May 31;106(5B):37S-42S. doi: 10.1016/s0002-9343(99)00115-1. PMID: 10390126. https://pubmed.ncbi.nlm.nih.gov/10390126/.
4 Rauf, Abdur et al. “Reactive oxygen species in biological systems: Pathways, associated diseases, and potential inhibitors-A review.” Food Science & Nutrition vol. 12,2 675-693. 1 Dec. 2023, doi:10.1002/fsn3.3784.
www.ncbi.nlm.nih.gov/pmc/articles/PMC10867483/.
5 Van Bogart, Karina et al. “The Association Between Loneliness and Inflammation: Findings From an Older Adult Sample.” Frontiers in Behavioral Neuroscience vol. 15 801746. 11 Jan. 2022, doi:10.3389/fnbeh.2021.801746. www.ncbi.nlm.nih.gov/pmc/articles/PMC8787084/.
6 Quirk, M. (2021). 5 exercises to ease chronic pain with gratitude. Psychology Today online. Retrieved May 29th, 2024. www.psychologytoday.com/ca/blog/ease-pain/202112/5-exercises-ease-chronic-pain-gratitude.
7 Brusewitz, J. & Coleman, K. (2020). Joint pain, alcohol, & NSAIDS: Harnessing the power of our plant allies. Retrieved May 29th, 2024. https://ndnr.com/autoimmuneallergy-medicine/joint-pain-alcohol-nsaids-harnessing-the-power-of-our-plant-allies/.
8 Worden, D. (2018). Homeopathic injection therapy treatment of chronic pain, depression, and fatigue. Retrieved May 29th, 2024. https://ndnr.com/homeopathy/homeopathic-injection-therapy-treatment-of-chronic-pain-depression-and-fatigue/.
Dr. Serena Goldstein is a naturopathic doctor in South Florida (in-person, and virtual world-wide available), who helps guide patients to trust and understand their body’s signs and signals so they can expand their knowledge and become partners on their health journeys. Dr. Goldstein utilizes conventional and natural medicine, psychology and intuitive healing to help patients achieve long-term weight loss, hormone balance, mood concerns, gut health and thyroid issues so they can bring order to chaos in wanting to feel more deeply connected to their health. Additionally, she treats all concerns with an individualized plan that her patients find fun, a source of motivation and a unique opportunity to learn more about their body than ever before.